For the first time, the Bank of Korea and the National Health Insurance Service have quantified the physical pain experienced by life-sustaining treatmentA procedure that only prolongs life when recovery is nearly impossible. patients.
The results revealed that the reality of life-sustaining treatment, which many of us vaguely understood, is far heavier and more agonizing than we imagined.
While many elderly people say, "If recovery is impossible, I do not want life-sustaining treatment,"
in actual end-of-life medical settings, these personal choices are not sufficiently reflected.
Researchers warned that if this gap is not addressed, not only will patient dignity be at risk,
but the economic and psychological burdens on families, as well as social costs, could also increase.
"We must focus on the pain experienced by patients"
(Pain Index → Life-sustaining Treatment Rate → Family & Social Burden)
World's First 'Life-Sustaining Treatment Pain Index'... Top 20% Suffer 12.7 Times More Pain
The research team developed the world's first 'Life-Sustaining Treatment Pain IndexAn indicator that scores the pain accumulated from multiple life-sustaining procedures.'.
This index demonstrates that the burden of life-sustaining treatment is on a completely different level from the pain felt in a single disease or single procedure.
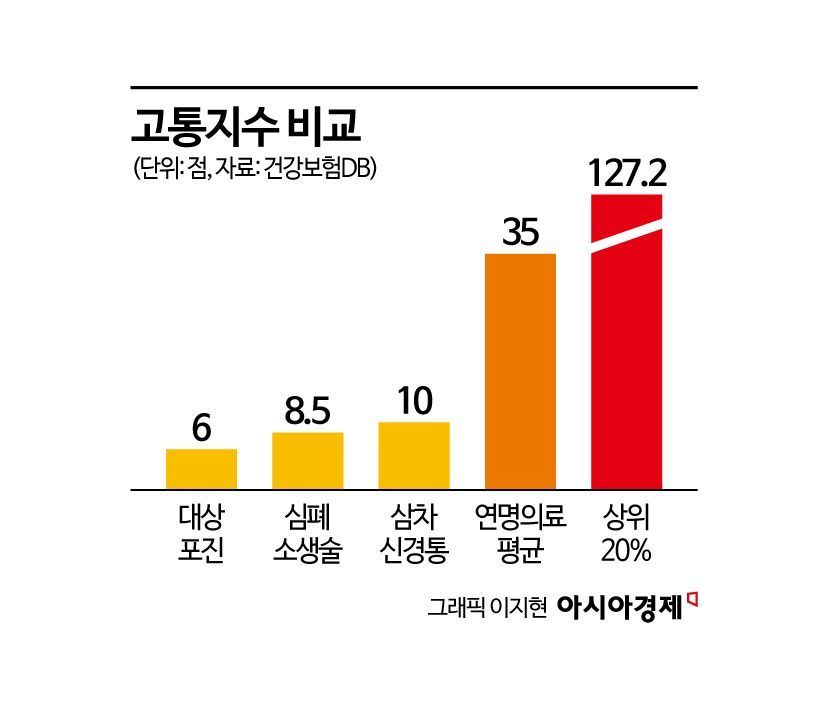
The average pain score for patients receiving life-sustaining treatment was 35 points.
This is about 3.5 times higher than the scores for severe pain such as shingles (6 points), cardiopulmonary resuscitation (8.5 points), or trigeminal neuralgia (10 points).
Notably, patients in the top 20% of the pain index scored 127.2 points, experiencing 'extreme pain' that is 12.7 times greater than what can be explained by single-disease standards.
This index was calculated by combining the intensity and frequency of pain from seven types of legally defined life-sustaining procedures, such as cardiopulmonary resuscitation, chemotherapy, mechanical ventilation, and extracorporeal life supportA procedure that replaces heart and lung function with an external machine..
Considering that patients themselves are often unable to respond,
the values were 'conservatively' estimated based on the experiences of patients who recovered after life-sustaining treatment.
Therefore, the actual pain may be even higher than these estimates.
"Unwanted Life-Sustaining Treatment Continues"
The study also reveals another important fact.
There is a significant gap between patient preferences and actual medical practice.
84.1% of seniors aged 65 and older said, "If recovery is impossible, I do not want life-sustaining treatment,"
but only 16.7% of actual deceased patients had life-sustaining treatment withheld or withdrawn.
This means that most elderly patients receive life-sustaining procedures until just before death, regardless of their wishes.
This discrepancy is the result of a combination of institutional factors, including lack of prior discussion, accessibility of ethics committeesOrganizations within hospitals that assist in decision-making about life-sustaining treatment., and the difficulty of determining the end-of-life stage.
In many cases, the decision to discontinue treatment is made only at the very end, resulting in a recurring conflict between the purpose of life-sustaining treatment and the patient's quality of life.
The Burden on Patients and Families Increases... Social CostsMedical, caregiving, and insurance expenditures borne by society due to life-sustaining treatment. Are Also Soaring
Life-sustaining treatment greatly increases not only the psychological burden on patients and families, but also actual expenses.
Out-of-pocket medical expenses for life-sustaining treatment patients during the final year of life rose from 5.47 million won in 2013
to 10.88 million won in 2023, doubling in just ten years.
This amount is equivalent to about 40% of the median income for households aged 65 and older.
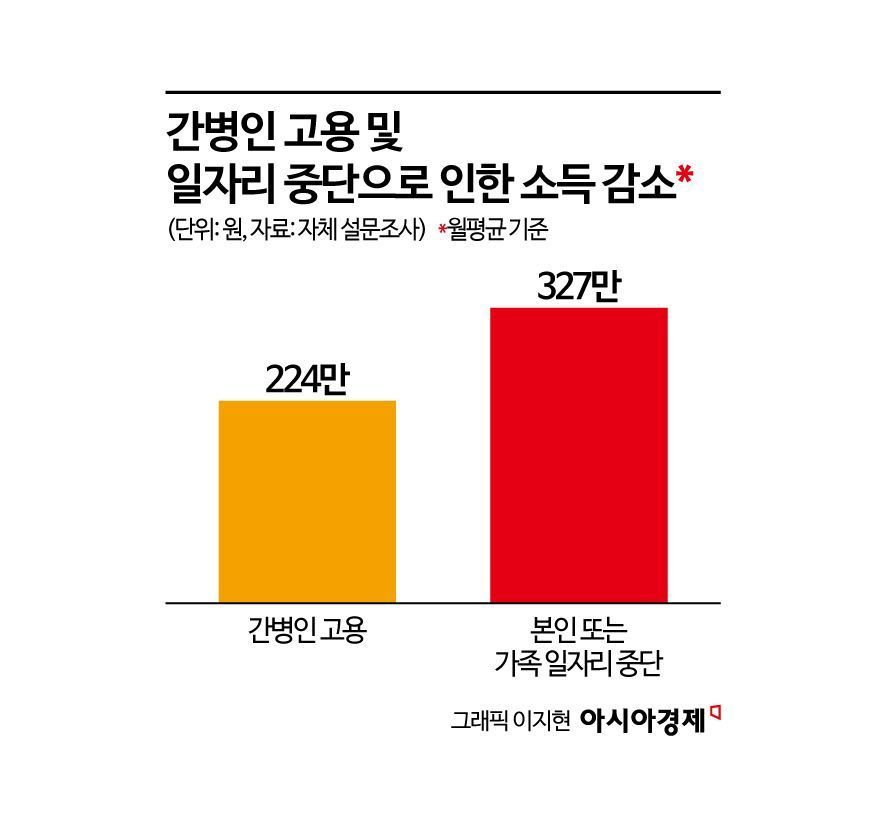
When factoring in caregiving costs and lost income, the burden becomes even greater.
The rate of increase in social costs is also steep.
If the current structure-where about 70% of elderly deaths involve life-sustaining procedures-continues,
health insurance expenditures for life-sustaining treatment are projected to reach about 3 trillion won in 2030 and 16.9 trillion won in 2070.
On the other hand, if patient preferences are properly reflected and the rate of procedures drops to around 15%,
expenditures could fall to about 3.6 trillion won, and the savings could be used to expand hospice and care infrastructure, according to the analysis.
"We must be able to record patient preferences more specifically"
(Expand items in Advance Directives for Life-Sustaining Treatment)
To ensure that patient wishes are respected in actual medical settings, the Advance Directive for Life-Sustaining TreatmentA document in which you specify in advance which life-sustaining treatments you wish to receive or refuse. must be further personalized,
and the selection items need to be subdivided. Researchers agreed on this point.
The current form requires an 'all-or-nothing' choice regarding the discontinuation of life-sustaining treatment,
so it does not sufficiently reflect the patient's values, religious beliefs, or preferences for specific procedures.
As a result, when the end of life approaches, it is difficult for medical staff and families to clearly understand the patient's intentions,
leading to repeated situations where unwanted life-sustaining treatment is administered.
The newly proposed form enables much more precise expression of patient intent.
▲ Selective refusal for each legally defined life-sustaining procedure
▲ Decision on artificial nutrition
▲ Organ donation intent
▲ Designation of a healthcare proxy
▲ Free-writing items such as preferred place of death and type of care
The core of this reform is not to 'reduce life-sustaining treatment,'
but to ensure that patient choices are genuinely respected until the very end of life.
Researchers especially emphasized the need to strengthen institutional and financial support so that patient autonomy can be realized even in small and medium-sized hospitals and nursing hospitals.












![[Reportage]"It Only Leads to Arguments"... Chungnam's True Sentiments Hide Deeper After Martial Law](https://cwcontent.asiae.co.kr/asiaresize/304/2026051223490460082_1778597344.jpg)
