"Fake Medical Bills to Be Detected by AI"... Crackdown on False and Fraudulent Health Insurance Claims Strengthened
Ministry of Health and Welfare to Conduct Intensive Investigations in Second Half of Year
AI Detection System Introduced... Fines Increased Up to Fivefold
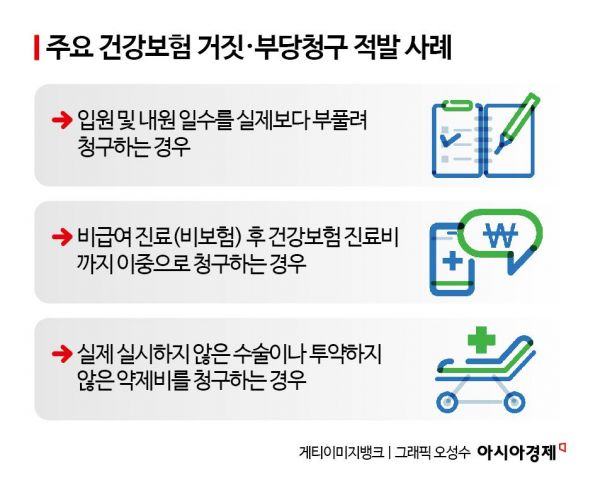
The government is strengthening its measures against false and fraudulent claims for medical care benefits by healthcare institutions in order to prevent financial leakage in the National Health Insurance system. The authorities will establish an AI-powered monitoring system and significantly raise the level of penalties, including fines of up to five times the illicit amount detected.
On April 23, the Ministry of Health and Welfare announced that it will expand its investigative workforce in the second half of this year and conduct intensive, targeted investigations into false and fraudulent health insurance claims. In addition to the current regular audits—conducted at about 45 institutions per month, or an average of 540 per year—the ministry plans to focus its analysis and investigations on types of claims with a high likelihood of fraud or a significant amount of detected false claims.
To enhance the accuracy of detecting fraudulent claims, the Health Insurance Review & Assessment Service will implement an AI-based fraudulent claims detection system. The AI will analyze vast amounts of medical data to identify abnormal patterns in advance, thereby improving the effectiveness of investigations.
For institutions found to have made false or fraudulent claims, the authorities will recover the illicit gains and may also impose a work suspension of up to one year. The fine imposed in lieu of a work suspension will be raised to up to five times the total fraudulent amount. For example, if a medical institution illicitly claims 2 billion won, the authorities could levy a fine of up to 10 billion won, meaning a total of 12 billion won would be collected.
In addition to legal action as prescribed by relevant laws, medical institutions that have made false claims exceeding 15 million won or whose false claims account for more than 20% of total claims will have their violations disclosed to the public following a resolution by the Health Insurance Public Disclosure Review Committee. Furthermore, institutions that refuse legitimate on-site investigations will face additional measures, such as enhanced monitoring and reinvestigation, in addition to a one-year work suspension, to ensure the effectiveness of the sanctions.
Institutions will also be encouraged to conduct voluntary self-checks and take preventive actions to correct fraudulent claims on their own. If a medical institution voluntarily reports a wrongful claim made due to a simple mistake through a self-audit, the illicit gains will be recovered but administrative penalties will be waived. In addition, monitoring will be conducted for five years after the self-audit to strictly manage any recurrence.
The ministry will also step up publicity regarding the "up to 3 billion won whistleblower reward" system, which was introduced last year, to activate a nationwide social surveillance network. Previously, the maximum reward differed between the general public and internal staff at healthcare institutions, but now anyone who reports can receive up to 3 billion won.
Hot Picks Today
 "I Want to Be as Beautiful as Korean Women": Fo...
"I Want to Be as Beautiful as Korean Women": Fo...
- "If You Have This at Home, Remove It Immediately"... 'This Item' Is as Harmful a...
- Trump Claims 'Division in Iran'... Mojtaba Calls Media Operation 'Malicious Inte...
- KOSPI Hits All-Time High, but "Why Is My Account Like This?"... Numerous Compani...
- "I Spent Money in a Truly Meaningful Way"... How an SK hynix Employee Donated 10...
Kwon Byungki, Director-General of Health Insurance Policy at the Ministry of Health and Welfare, stated, "We will establish a culture of legitimate claims by conducting effective investigations and imposing penalties to ensure that no unnecessary leakage occurs in the National Health Insurance, which is funded by the precious contributions of the people. We will also provide opportunities for institutions to improve on their own and will actively pursue incentives at the review stage for exemplary institutions."
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.