War on Insurance Fraud... Even Launching a YouTube Channel
Life Insurance Association Promotes 'Insurance Fraud Out' Channel
Serious Organization of Fraud Crimes Involving Hospitals and Agents
Raising Awareness with Various Cases of Dosu Treatment and Alveolar Bone
[Asia Economy Reporter Oh Hyung-gil] "An insurance agent encouraged me to sign up for insurance by saying that I could receive insurance money just by being hospitalized. The agent said I only needed to be admitted to a hospital they designated. Is this insurance fraud?"
The Life Insurance Association recently rolled up its sleeves to promote its newly launched YouTube channel to insurance companies and related institutions. Their methods to increase subscribers are no different from typical YouTubers. They explain each step of how to subscribe in detail. Why did the association create a YouTube channel amid the flood of diverse content on YouTube?
The channel opened by the Life Insurance Association is called "Insurance Fraud Out." It features web drama-style videos around 10 minutes long. As the name suggests, it depicts the Insurance Fraud Investigation Unit (SIU) task force investigating and uncovering insurance fraud. Videos for season 2 have already been uploaded.
Starring task force members, the channel clearly explains various cases occurring in the insurance field, from false and excessive treatments such as cataracts, physical therapy, and alveolar bone, to fraud involving insurance agents and other insurance-related personnel. It also includes information that reporting insurance fraud can lead to rewards.
An association official explained, "There are frequent cases where people get involved in insurance fraud just by trusting what hospitals or agents say," adding, "We created the YouTube channel to raise awareness through examples showing that actions done unknowingly can turn into insurance fraud."
The association’s unusual move to launch a YouTube channel is a last-ditch effort to eradicate the increasing insurance fraud cases day by day.
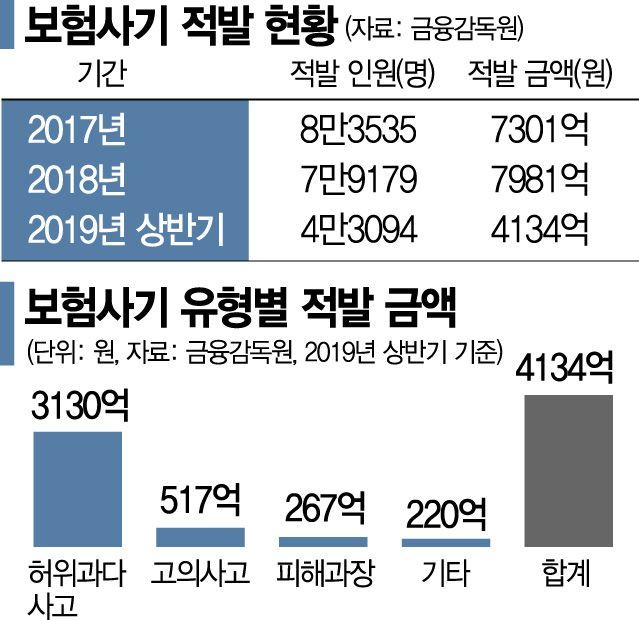
According to the Financial Supervisory Service, the amount detected for insurance fraud was 413.4 billion KRW in the first half of last year, an increase of 13.4 billion KRW compared to 400 billion KRW in the same period the previous year. In the first half of 2017, it was 370.3 billion KRW, showing a trend of increasing by hundreds of billions of KRW annually. The number of people caught for insurance fraud in the first half of last year was 43,094, up 11.4% from the previous year.
While hard frauds, such as intentional accidents like injury or self-harm, are decreasing, soft frauds involving manipulation of accident details or exaggeration of damages are increasing. Insurance fraud methods are also becoming increasingly sophisticated and cunning.
There is a tendency toward organization involving not only doctors but also insurance agents and brokers. Recently, platforms like YouTube, Instagram, and Facebook have been exploited as tools for insurance fraud. Content that misleads viewers, such as how to claim more insurance money or how to negotiate insurance settlements well, is overflowing and encouraging insurance fraud.
The insurance industry is so committed to reducing insurance fraud that it has even developed detection systems applying big data and artificial intelligence (AI) technology. However, there are criticisms that industry efforts alone have limitations.
The insurance industry is primarily demanding amendments to the Special Act on the Prevention of Insurance Fraud. They argue that a cooperative system should be established among public insurance-related institutions such as the National Health Insurance Service and the Health Insurance Review & Assessment Service, along with insurance companies, to activate insurance fraud investigations and establish recovery provisions.
Hot Picks Today
 Taking Annual Leave and Adding "Strike" to Profiles, "It Feels Like Samsung Has Collapsed"... Unsettled Internal Atmosphere
Taking Annual Leave and Adding "Strike" to Profiles, "It Feels Like Samsung Has Collapsed"... Unsettled Internal Atmosphere
- There Is a Distinct Age When Physical Abilities Decline Rapidly... From What Age Do Strength and Endurance Drop?
- "One Comment Could Lead to a Report": 86% of Elementary Teachers Feel Anxious; Half Consider Resignation or Career Change
- "After Vowing to Become No. 1 Globally, Sudden Policy Brake Puts Companies’ Massive Investments at Risk"
- On Teacher's Day, a Student's Gifted Cake Had to Be Cut into 32 Pieces... Why?
An industry insider emphasized, "The procedure from reporting to reward payment should be unified to encourage insurance fraud reporting," adding, "It is also necessary to strengthen reward payment criteria to induce internal whistleblowers such as medical personnel and agents to report."
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.