"I Thought It Was Cancer"...Stoking Patient Anxiety Backfires as Deferred Judgments Are Reined In Within Three Months
NHIS finds wide variation in deferred-judgment rates by institution, up to 93%
Top 100 high-rate institutions cut unnecessary re-examinations such as ultrasound by 3,155 cases
By intensively monitoring hospitals and clinics with unusually high rates of re-examination recommendations in X-ray screenings for breast cancer, about 350 million won of National Health Insurance funds were saved over three months.
The National Health Insurance Service (NHIS) announced on the 12th that it had conducted an investigation into screening institutions with excessively high rates of deferred judgments in order to improve the accuracy of breast cancer screenings and reduce unnecessary re-examinations, and that this led to improvements in diagnostic accuracy and savings in insurance spending.
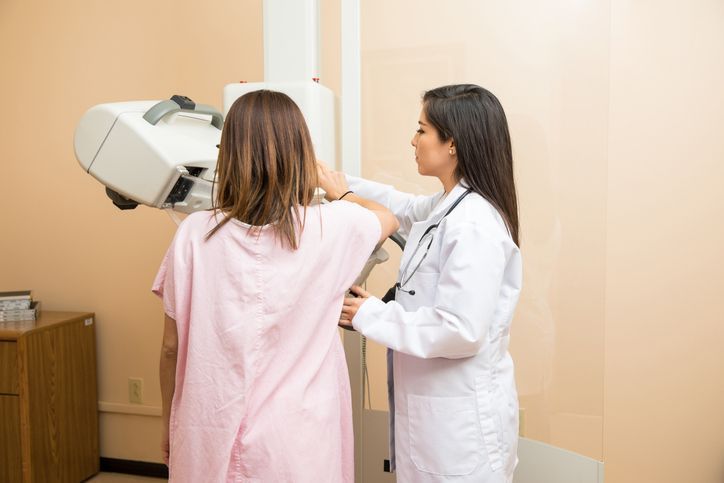
By intensively monitoring hospitals and clinics with unusually high rates of re-examination recommendations in X-ray screenings for breast cancer, about 350 million won of National Health Insurance funds were saved over three months. Photo by Getty Images
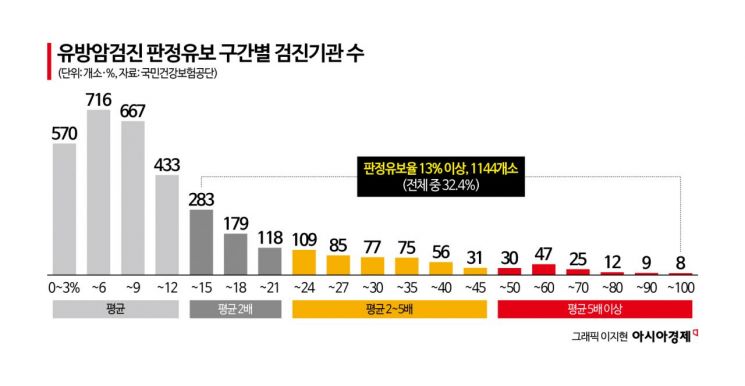
View original imageAccording to an analysis by the NHIS, among approximately 4.5 million people who underwent breast cancer screening in 2024, 69.9% (3,191,000 people) were classified as "no abnormal findings," 19.0% (867,000 people) as having "benign disease," 0.2% (8,000 people) as "suspected cancer," and 10.9% (500,000 people) as "deferred judgment." A deferred judgment means that the image is insufficient and a retake is required, or that there are abnormal findings that necessitate additional tests such as breast ultrasound.
Looking at the trend in breast cancer screening results over the past six years, the proportion of "no abnormal findings" slightly decreased from 72.1% in 2019 to 69.9% in 2024, while during the same period, the proportion of "benign disease" increased from 16.0% to 19.0%. The NHIS explained that diagnostic accuracy is crucial, given that about 8,000 patients suspected of having cancer are identified each year through screening.
However, in some clinical settings, there appears to be a tendency to overuse ambiguous deferred judgments, citing reasons such as "dense breasts." When breast cancer screening deferred-judgment rates were compared across different screening institutions, the lowest rate was only 1.6%, whereas at the highest, 92.9% of examinees were classified as deferred judgments, indicating an extreme disparity.
In response, in September last year the NHIS carried out on-site and written investigations targeting the top 100 screening institutions with the highest deferred-judgment rates. During the investigation, the NHIS recommended that these institutions thoroughly implement quality control to reconfirm the criteria for diagnosing dense breasts and to improve diagnostic accuracy. Quality control refers to systematically managing the entire pre- and post-analysis process of health examinations, including sample collection, analysis, and data processing, in order to detect and prevent errors at an early stage and thereby ensure accuracy and reliability.
Tracking changes over the three months following the investigation, the average deferred-judgment rate at these institutions plunged by 24.1 percentage points, from 66.8% to 42.7%. As a result, the number of people receiving deferred judgments decreased by 3,155, and the associated costs of breast ultrasound examinations were estimated to have been reduced by 352 million won.
Hot Picks Today
NHIS President Jeong Kiseok said, "Through this investigation, we confirmed that analyzing the causes and strengthening management at screening institutions with high deferred-judgment rates can in fact lead to improved diagnostic accuracy and savings in National Health Insurance finances," adding, "We will continue to reinforce evidence-based quality management so that the public can trust and use the national screening services."
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.