If You Worry About Antibiotic Resistance... 'Gudeogi Therapy' Regains Spotlight for Treating Intractable Wounds
by Kim Hyunjeong2
Published 05 Nov.2022 12:00(KST)
Cases of maggot therapy in the UK increased by 50% over 10 years
U.S. Food and Drug Administration (FDA) recognizes maggots and leeches as 'medical devices'
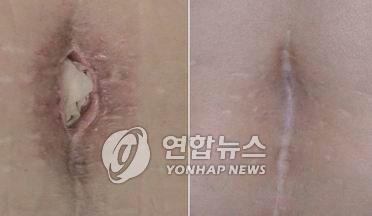
A scene of maggot therapy being applied to a wound that had not healed (left) and the healed wound after maggot therapy. Photo by Yonhap News Agency
View original image[Asia Economy Reporter Kim Hyunjung] In the UK, cases of maggot therapy, which uses maggots to treat intractable wounds, have increased by 50% over the past decade.
On the 3rd (local time), the UK Telegraph reported that maggot therapy is gaining renewed attention as wound treatment becomes more difficult due to increasing antibiotic resistance. According to statistics from the UK's National Health Service (NHS), the number of maggot therapy cases has been steadily rising since records began in 2007.
The number of wound treatments using maggots in the UK rose from 886 cases in 2008-2009 to 1,305 cases in 2018-2019, an increase of over 50%.
The Telegraph introduced the case of Biomonde, headquartered in South Wales, UK. This company breeds thousands of green bottle flies annually for sale to the NHS and across Europe, supplying the NHS with 9,000 maggot-filled tea bags each year. Maggot therapy is used as a "last resort" to treat wounds that do not heal with antibiotics. The method involves placing a tea bag filled with maggots smaller than 1mm on the wound, covering it with a dressing, and leaving it for up to four days. The maggot larvae consume dead tissue from the wound, and some studies suggest they secrete antimicrobial substances that disinfect the wound. The inflammatory exudate and dead cells produced at the wound site serve as good food for the maggots, and the digestive enzymes of the maggots contain antimicrobial substances such as defensins and serratins, making maggot therapy an effective treatment that benefits both humans and maggots?a true "win-win" therapy.
The use of maggots for wound treatment has a long history. Modern medicine began using maggots for wound care during World War I, but even earlier, in the late 18th century, Dominique Jean Larrey, Napoleon’s chief surgeon, reportedly treated wounds with maggots during Napoleon’s Egyptian campaign. Maggot therapy lost popularity after the widespread use of antibiotics from the 1940s onward but has recently regained attention due to the rise of antibiotic-resistant patients for whom antibiotics are ineffective. Additionally, this therapy is cost-effective. In the UK, maggot therapy is covered by health insurance.
Medical professionals’ reactions to maggot therapy are polarized. Wound care specialist nurses who have directly experienced the treatment’s effectiveness and benefits highly prefer this therapy,
while general nurses without wound care specialization tend to avoid maggot treatment. Yamni Nigam, a professor of health care at Swansea University, said, "Clearly, most people have an innate aversion to crawling insects, and healthcare professionals are likely to feel even greater disgust toward maggot therapy than patients. However, this stems from a lack of trust in the treatment and can be alleviated through training and education."
Besides maggots, leeches are also used to treat diseases with insects. The U.S. Food and Drug Administration (FDA) recognizes both maggots and leeches as "medical devices," and in South Korea, medical leeches were introduced in the late 1990s and are widely used during surgeries to improve blood circulation and reduce pain. The use of leeches for disease treatment dates back a long time, as mentioned in the 1613 medical text Donguibogam compiled by Heo Jun, which discusses leech bloodletting therapy.