AI Prescriptions Tested in 'Virtual Hospital' for Impact on Patient Outcomes and Bed Shortages
by Jo Inkyung
Published 14 Apr.2026 15:00(KST)
Seoul National University Hospital and Harvard Medical School Unveil World’s First Medical AI Simulator, ‘CES’
Moving Beyond Historical Data to Real-Time Tracking of ‘Cascading Effects’ in Clinical Settings
Moving beyond the traditional, fragmented evaluation of medical artificial intelligence (AI) through written tests based solely on historical data, a world-first model has now been unveiled that allows AI to be tested in a virtual hospital environment that mirrors real clinical settings. This approach makes it possible to preemptively verify the cascading effects of AI prescriptions not only on patient outcomes but also on the depletion of hospital resources. Experts say this opens a rigorous preclinical stage to thoroughly assess safety before applying AI to actual patients.

Sung Eun Kim, Research Professor at the Specialized Research Institute, Seoul National University Hospital Biomedical Research Institute. Seoul National University Hospital
원본보기 아이콘On April 14, a joint research team led by Research Professor Sung Eun Kim at the Specialized Research Institute of Seoul National University Hospital and Harvard Medical School announced the development of the 'Clinical Environment Simulator (CES),' a tool for dynamically evaluating medical AI based on large language models (LLMs).
Conventional medical AI evaluation has been limited to answering predetermined questions using fixed historical data. However, in real hospitals, patient conditions change continuously, and each physician order directly affects the consumption of limited resources such as beds and staff. Thus, previous methods were unable to assess such temporal and systemic interdependencies. In response, the research team argued that, just as pilots train in flight simulators, medical AI must also be evaluated for its adaptive capabilities over time and under resource constraints.
To implement this, the team synchronized two core engines. First, the 'patient engine' uses disease trajectory templates defined by medical specialists and initial patient data from electronic medical records. The LLM then dynamically generates a variety of simulated symptom and treatment response pathways, modeling how a patient's condition evolves.
Working in tandem, the 'hospital engine' faithfully reproduces step-by-step work processes in real hospitals based on actual time data, tracking bed availability, medical staff, and equipment status in real time. For example, when a blood test is ordered, the necessary medical personnel are sequentially allocated according to the actual time required for each step. The system also incorporates a realistic prioritization mechanism that allocates resources preferentially to critically ill patients.
In this virtual hospital, crisis situations are vividly simulated depending on the timing of AI intervention. For instance, if the AI delays ordering a test, a patient with stable chest pain could deteriorate into acute myocardial infarction. Conversely, if the AI assigns priority access to critical resources like CT scanners to one emergency patient, other patients may face lengthier wait times, creating realistic bottlenecks. This system replicates how a single AI decision can determine the fate of an individual patient and exhaust available hospital resources, thereby sequentially limiting care opportunities for subsequent patients-just as in a real hospital environment.
Every AI decision is evaluated using a 'dual-indicator composite score' that integrates two axes: patient prognosis (survival, treatment duration, guideline adherence) and hospital operational efficiency (total hospital stay, emergency department throughput, utilization of beds and equipment). The system rewards improvements in care that do not undermine overall hospital performance, but penalizes excessive concentration of resources on one patient at the expense of others, enforcing a strict balance. Furthermore, it is stress-tested under extreme scenarios such as network outages and mass-casualty emergencies.
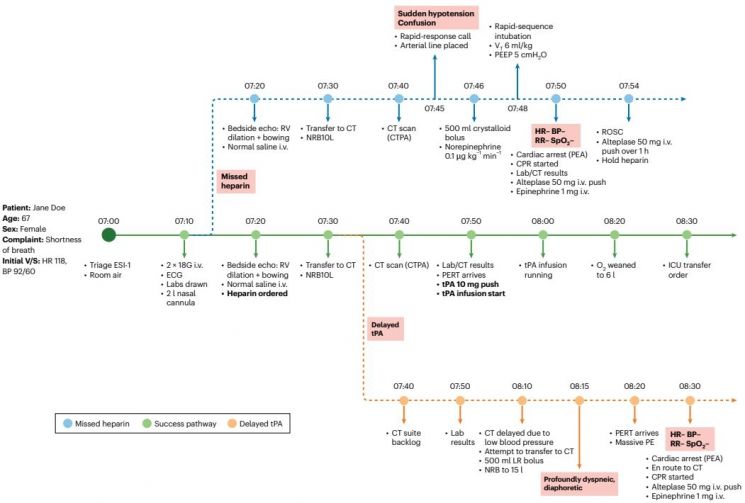
Dynamic patient condition changes over time. The simulation of ripple effects shows that the prognosis of critically ill patients diverges into three pathways depending on the timing of medical AI intervention (green: stabilization, blue and orange: condition deterioration). Seoul National University Hospital
원본보기 아이콘The core of this study lies in establishing a 'risk-free preclinical testing environment' that demonstrates system safety without exposing patients to harm. If thoroughly validated AI can act as a digital proxy for healthcare professionals and handle complex system operations, physicians can finally step away from their monitors and refocus on their essential roles of empathy and clinical judgment at the patient’s side.
Research Professor Sung Eun Kim (co-first author) commented, "While a virtual hospital cannot perfectly predict the complex physiological responses of the human body, this study represents the most valuable next step-verifying that medical AI can move beyond solving fragmented problems to become fully integrated within dynamic healthcare systems, offering real, practical assistance."
This research on the digital virtual hospital evaluation framework was published in the latest online edition of the international journal Nature Medicine (IF 50).
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.