COVID-19 Infection Confirmation ... How Do PCR and Rapid Antigen Tests Differ?
by Jo Inkyung
Published 30 Jan.2022 08:15(KST)
Highly Accurate Standard Testing Method vs Rapid Antibody Generation Confirmation
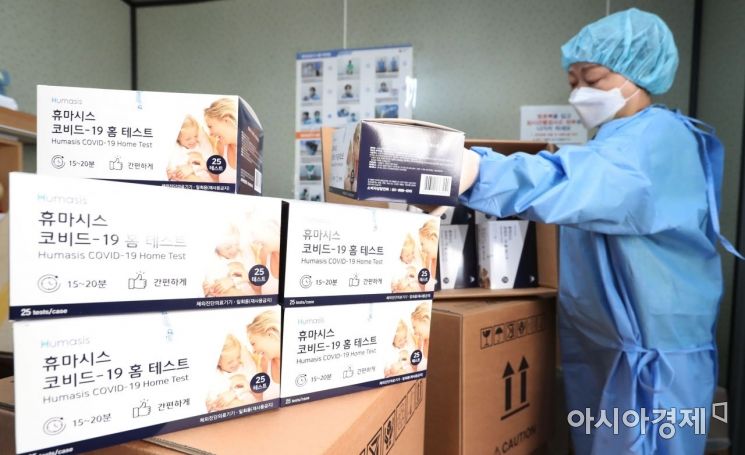
On the 28th, medical staff are organizing rapid antigen test kits at the temporary screening clinic at Seoul Station, where PCR tests and rapid antigen tests are set to be conducted simultaneously, focusing on COVID-19 screening clinics installed at public health centers and large hospitals nationwide. Photo by Hyunmin Kim kimhyun81@
원본보기 아이콘As rapid antigen testing using self-test kits that can quickly determine COVID-19 infection status expands, it has become important to understand the correct way to use these kits. In particular, if a rapid antigen test result is positive, it is essential to confirm the positive status by retesting with a 'nasopharyngeal swab polymerase chain reaction (PCR)' test. How does the self-test kit using the rapid antigen diagnostic method differ from the conventional PCR test?
If Positive on Self-Test Kit, Additional PCR Test Required
The PCR test, which has been used for COVID-19 diagnosis in Korea, collects specimens by inserting a swab deep into the nasal cavity or the back of the throat. RNA (ribonucleic acid) is then extracted from the specimen, and if two or more genes characteristic of COVID-19 test positive after amplification, the case is confirmed as positive.
This method is quite accurate and is used as a global standard testing method, but it takes about six hours to confirm infection status, which reduces its speed. Also, if an insufficient amount of virus cells is collected during specimen collection, the test may show a negative result even if the person is infected.
On the other hand, the rapid antigen test detects the presence of components such as proteins that make up the COVID-19 virus in specimens collected from the nasopharynx. While the PCR test examines the virus itself in infected cells, the antibody test checks for antibodies produced by the body's immune response when the COVID-19 virus enters the body. If antigens are detected in the specimen, it is considered positive, indicating a presumed infection.
Like existing influenza or pregnancy tests, this simple test method shows two lines in the test window to indicate a positive result, and results can be confirmed within 30 minutes. However, since the test is conducted without specimen amplification, if the amount of virus is low, the result may be negative, and depending on the timing of specimen collection, sensitivity can vary significantly, leading to the possibility of false negatives, known as 'false negatives.'

The video titled 'Proper Usage and Guidelines for COVID-19 Self-Test Kits' released by the Ministry of Food and Drug Safety on YouTube.
원본보기 아이콘Swab 1.5~2 cm Deep into Nostril, Swabbed More Than 10 Times
Currently, three types of rapid antigen COVID-19 self-test kits are officially approved by the Ministry of Food and Drug Safety and distributed in Korea: SD Biosensor, Humasis, and Rapigen products. Although the swab (sterile swab) length and disposal bag size differ slightly, the basic components and usage methods are similar.
To perform the test using the self-test kit, first wash your hands and wear disposable gloves to prevent contamination of the swab and tube. Then, insert the swab about 1.5 to 2 cm into each nostril in turn and swab in a circular motion about 10 times to collect nasal mucus specimens from the nasal cavity.
Place the swab with the specimen into the extraction tube containing reagent and mix it. Then, squeeze the sides of the tube to extract the specimen from the swab and remove it, and close the tube with the nozzle cap. Next, hold the tube upside down and drop 3 to 4 drops of the specimen mixture onto the test device. Shortly after, a single control line C will appear in the result window. If only the control line remains after waiting about 15 to 30 minutes, the result is 'negative'; if a test line T also appears, showing two lines, the result is 'positive.'
If the result is positive, an additional PCR test must be taken. Even if the result is negative immediately, the possibility of a false negative cannot be excluded, so until the final result is confirmed, hygiene rules such as wearing a mask should be followed to prevent infection.
© The Asia Business Daily(www.asiae.co.kr). All rights reserved.